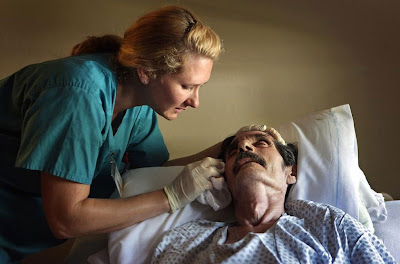
I first proposed developing an end of life care team in January, and while my nurse manager and others have been completely supportive from the start, it's taken until today to get the official word out to colleagues with this announcement and recruitment email:
Hi Folks:It's a big moment for me, personally and professionally.
This is a lengthy email, but here are a couple of quick questions to decide if you should continue reading it -
1.Do you want to develop or enhance your you current skills in caring for patients and families at the end of life (EOL) as a central part of your clinical practice on 9C/D?
2.Will you commit to actively participating in a series of half-day educational programs to develop your EOL care skills?
This commitment will require you to read on different topics from a variety of sources in preparation for the sessions, actively participate in workshop exercises and group discussions, and engage in self-reflection through writing and story telling.
The expected outcome will be that you will be capable of providing expert EOL care; review and assess current policies regarding EOL care; help develop new policies and tools to improve EOL care on 9C/D; and be a visible and active resource to our colleagues regarding EOL care."The End-of-Life Nursing Education Consortium (ELNEC) project is a national education initiative to improve end-of-life care in the United States. The project provides undergraduate and graduate nursing faculty, CE providers, staff development educators, specialty nurses in pediatrics, oncology, critical care and geriatrics, and other nurses with training in end-of-life care so they can teach this essential information to nursing students and practicing nurses. The project, which began in February 2000, was initially funded by a major grant from The Robert Wood Johnson Foundation (RWJF). Additional funding has been received from the National Cancer Institute (NCI), the Aetna, Archstone, and California HealthCare Foundations, Open Society Institute, and the Oncology Nursing Foundation."Jerry, a qualified ELNEC trainer, will direct a series of 3 four-hour sessions starting in the coming months to develop an EOL nursing care team specifically for 9C/D patients, families and fellow staff. The educational program is based on the ELNEC curriculum.
You can learn more about ELNEC here.
As a member of the 9C/D EOL Care Team following your training, you will provide direct EOL care to patients and families and also be a visible and active resource to colleagues when you are not directly assigned to a patient and family at EOL.
You will help with the early identification of potential ethics consults, and provide monitoring and follow-up on patients who die on 9C/D on behalf of the New England Organ Bank, the Bereavement Committee, and other related groups here.
Finally, you will help assess and develop tools, policies, and practice standards for EOL care on 9C/D; and help improve the overall quality and effectiveness of the EOL care we provide on our unit.
Jerry developed this project as a result of his own clinical interest in caring for patients and families at end of life, and based on his qualifications and professional development.
Jerry has been a nurse for 33 years. He earned a diploma in nursing from Catholic Medical Center in Manchester, NH in 1976; a bachelor of science in nursing from Boston State College (now Umass/Boston) in 1981; and a graduate certificate of special studies (CSS) in health policy from Harvard University in 1987. He is currently enrolled in the master of science in nursing program at St. Joseph's College in Standish, Maine.
Since 2002, his professional development has focused exclusively on EOL care through programs and training at Beth Israel Deaconess Medical Center, the MGH Institute, the Harvard Medical School Center for Palliative Care, the Harvard Center for Bioethics, and ELNEC.
Jerry's 14 years of clinical experience in critical care and hemodialysis has brought him into frequent contact with patients and families at end of life. He also spent 19 years in the information technology field, working with computer systems in clinical settings.
Jerry became an ELNEC trainer in October, 2008
The ELNEC curriculum is divided into 9 distinct modules -
Module 1 - An Introduction to Palliative Care
Module 2 - Pain Assessment and Management
Module 3 - Managing Other Symptoms at End of Life
Module 4 - Ethical and Legal Issues
Module 5 - Cultural Considerations
Module 6 - Communication Skills for End-of-Life Nursing Care
Module 7 - Loss, Grief, and Bereavement
Module 8 - Achieving Quality Care at the End of Life
Module 9 - Preparation and Care at the Time of Death
ELNEC trainers can adjust the sequence and specific focus of the individual modules to meet the needs of the audience. The first half-day program for the 9C/D EOL care team will include the content from the modules on Ethics, Communication, and Grief/Loss to accommodate several non-nurses who have expressed an interest in attending that session.
The two subsequent sessions will focus on content from the other modules specific to nursing practice.
Each half-day program will include a mix of lecture, case studies, class discussions, and media presentations. You are expected to prepare by reading the essential materials; to actively participate in discussions; and continue your learning beyond the classroom through self-directed reading and research, and self-reflection via journaling and story-telling.
At the conclusion of the program you will be recognized as being ELNEC trained, which includes a special pin for your ID badge or scrub stop. Note that this is not a certification or credential, but it is an explicit acknowledgement of your accomplishment. You will also earn CEU's for 12 contact hours of approved content, and become an essential member of a team dedicated to improving and maintaining the quality of EOL care on our unit.
If you're still interested, please contact via email to me , with a copy to Vince and Jerry.
In your email, please describe your own interest, experience, and goals pertaining to end of life care. It will be very helpful for you to include a brief story about a case where you were called upon to provide EOL care. That experience can either be a positive or negative one. In either event, indicate what you learned from it.
In the meantime, if you have any questions or comments specifically about this program, please ask Jerry via email or in person. For any logistical questions please contact me.
This email will help me understand the level of interest and allow me to plan appropriately.
Thanks for reading through to this point, and for your consideration.
Shaun
And the Red Sox are looking pretty good heading into 2009 postseason play...
Update 10/2: Here's another reason for me to celebrate - I just got my first reader comment in quite a while!